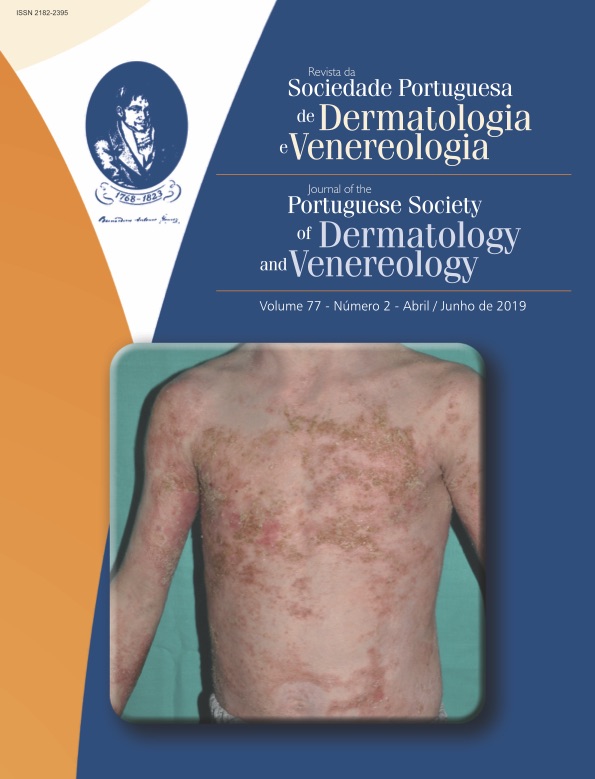
An Exuberant Case of Cutaneous Larva Migrans
Abstract
Cutaneous larva migrans (CML) is a dermatozoonosis characterized by a rash of erythematous lesions, usually prominent, papulo-vesiculous, linear or serpiginous, and most often pruritic. It is caused by penetration and intraepidermal migration of three possible species of nematode larvae. The highest rates of transmission occur in tropical coastal regions, where larvae can migrate freely in sandy soils and where hot temperatures and humidity are ideal for their viability. A case of a 51-year-old male patient who developed a pruritic skin rash on the back, flank, iliac fossa and lower limb on the right is reported. The injuries appeared about seven days after the practice of sport and leisure on turf field. After reviewing the scientific literature, we analyzed the epidemiological, parasitological, clinical, laboratory and therapeutic aspects inherent to the topic of cutaneous larva migrans. It is a common dermatological disease in tropical and subtropical countries, being very important its prompt recognition and therapeutic management for rapid cure with low morbidity.
Downloads
References
Kalil CLPV, Webber A. Zoodermatoses. In: Ramos-e-Silva M, Castro MC, editores. Fundamentos de dermatologia. Rio de Janeiro: Editora Atheneu; 2010. p.1055-6
Velho PE, Faria AV, Cintra ML, de Souza EM, de Moraes AM. Larva migrans: a case report and review. Rev Inst
Med. Trop S Paulo. 2003; 45:167-71.
Feldmeier H, Heukelbach J. Epidermal parasitic skin diseases: a neglected category of poverty-associated
plagues. Bull World Health Organ. 2009; 87:152-9.
Neto PB, Azulay RD, Azulay DR. Dermatozoonoses. In: Azulay RD, Azulay DR, Azulay- Abulafia L, editores.
Dermatologia. 5 ed. Rio de Janeiro: Guanabara Koogan; 2009. p. 445-446
Hochedez P, Caumes E. Hookworm-Related Cutaneous Larva Migrans. Travel Med. 2007; 14:326-33.
Caumes E. Treatment of cutaneous larva migrans. Clin Infect Dis. 2000;30:811-4.
Patel S, Sethi A. Imported tropical diseases. Dermatol Ther. 2009; 22: 538-49.
Bouchaud O, Houzé S, Schiemann R, Durand R, Ralaimazava P, Ruggeri C, et al. Cutaneous larva migrans in
travelers: a prospective study, with assessment of therapy with ivermectin. Clin Infect Dis. 2000; 31:493-8.
Ribeiro LC, Rodrigues Junior EN, Silva MC, TakiuchiII A, Fontes CJ et al. Púrpura em paciente com estrongiloidíase disseminada. Rev Soc Bras Med Trop. 2005; 38:255-7.
Te Booij M, de Jong E, Bovenschen HJ. Löffler syndrome caused by extensive cutaneous larva migrans: a case report and review of the literature. Dermatol Online J. 2010; 16:2.
Macias VC, Carvalho R, Chaveiro A, Cardoso J. Larva migrans cutânea – a propósito de um caso clínico. Rev
Soc Port Dermatol Venereol. 2013; 71: 93-6.
All articles in this journal are Open Access under the Creative Commons Attribution-NonCommercial 4.0 International License (CC BY-NC 4.0).